Fibromyalgia and Irritable Bowel Syndrome
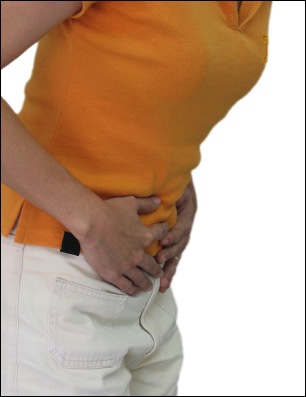 Irritable bowel syndrome is a disorder of the large intestine and causes severe and debilitating symptoms like cramping, bloating, diarrhea, constipation, gas, and abdominal pain. While it doesn’t cause changes to the tissues like inflammatory bowel disease does, it is still a chronic condition that needs long-term management. Experts report that nearly 10% to 20% of the population suffer from IBS, but millions go undiagnosed and untreated. Furthermore, up to 73% of patients with fibromyalgia have IBS.
Irritable bowel syndrome is a disorder of the large intestine and causes severe and debilitating symptoms like cramping, bloating, diarrhea, constipation, gas, and abdominal pain. While it doesn’t cause changes to the tissues like inflammatory bowel disease does, it is still a chronic condition that needs long-term management. Experts report that nearly 10% to 20% of the population suffer from IBS, but millions go undiagnosed and untreated. Furthermore, up to 73% of patients with fibromyalgia have IBS.
Diagnosing IBS requires certain symptoms to be present for at least 12 weeks over a period of 12 months. These do not need to be consecutive. Some patients will have constipation, some will have diarrhea, and others will fluctuate between the two. These are the most common symptoms of IBS, but it must also be associated with abdominal pain, and at least 2 of the following:
- Pain relieved with defecation
- Pain being associated with a change in the frequency of bowel movements
- Pain being associated with the form of the stool (i.e., watery or pellet like)
Serotonin plays a major role in the cause of IBS, and this neurotransmitter is dangerously deficient in nearly all fibromyalgia patients.
Current research shows that IBS is caused by a dysfunctional neuroendocrine immune system (the hormones in the brain and stomach). Serotonin is the main hormone that controls gut motility, or how fast/slow food moves through the intestines. Actually, 90% of serotonin receptors are in the gastrointestinal tract… not the brain.
It’s thought that depleted serotonin levels leads to hypersensitive receptors in the GI tract, which is why so many fibromyalgia patients suffer with IBS. This may also explain why people with IBS (even those who don’t have fibromyalgia) suffer with anxiety or depression. In fact, research has found that 54% to 94% of people with IBS meet clinical criteria for anxiety, depression, and/or panic disorders.
 Most IBS patients are taking a prescription medication like a smooth muscle relaxant, antidepressant, anti-diarrheal, or bulk-forming laxatives, all of which can endanger your life and well-being.
Most IBS patients are taking a prescription medication like a smooth muscle relaxant, antidepressant, anti-diarrheal, or bulk-forming laxatives, all of which can endanger your life and well-being.
Let’s take a closer look at some of the medications used for IBS patients.
Zelnorm (tegaserod) was once used for constipation-predominant IBS. This was the “miracle drug” for this condition. In previous posts and books, I warned of the side effects that come with this drug, and now it’s been removed from the market because of its association with stroke and heart attacks. There were still other potential side effects that experts were warning people about including liver damage, kidney impairment, adhesions, bowel obstruction, back pain, and gallbladder disease. The percentage of people who experienced life-threatening side effects was 10 times higher than those on the placebo.
Lotronex (alosetron) was the main drug of choice for diarrhea-predominant IBS. This drug was also removed from the market (though for only a short period of time) because within a few months of it coming out, there were reports of ischemic colitis (a condition that happens when blood supply to the intestines is blocked). Many reported major constipation and severe abdominal pain. This drug was responsible for at least four deaths, too. Lotronex has been put back on the market with stricter prescribing guidelines.
Antispasmodics like Levsin and Bentyl are routinely prescribed for IBS. Side effects are both severe and likely and include blurred vision, bloating, constipation, clumsiness, dizziness, diarrhea, difficulties breathing, drowsiness, vomiting, nervousness, rash, chest tightness, pounding in the chest, swelling, irregular heartbeat, fainting, memory loss, muscle pain, insomnia, and weakness.
 IBS is a symptom, not a disease! A poorly functioning digestive, elimination system is a warning sign (a symptom) of poor diet, too much stress, and depleted stress coping chemicals.
IBS is a symptom, not a disease! A poorly functioning digestive, elimination system is a warning sign (a symptom) of poor diet, too much stress, and depleted stress coping chemicals.
By changing your diet, reducing your stress (getting deep restorative sleep), and replenishing depleted stress coping the symptoms of poor digestion and elimination are corrected
Normal bowel activity is at least one stool every 24 hours, which should be soft but formed; however, one bowel movement after each meal is ideal, and you can get this using much less dangerous, natural supplements.
Without getting into too much detail about natural ways to treat IBS (which I will cover in another post), I will mention that patients who are on my CFS/Fibro Formula, 5HTP, along with a digestive enzyme, find their bowels are normalized within a couple of weeks. This formula contains a healthy dose of magnesium, which is a natural relaxant and will relax the colon sufficiently. Usually, 700 mg is what you want to aim for in magnesium, though some people need more or less to have soft, formed stools. They should never be loose, however, so if bowels become loose, you have too much magnesium (simply decrease your dose).
For loose BMs, combine 5HTP, magnesium, and digestive enzymes to correct any low serotonin states. You have more serotonin receptors in your intestinal tract than you do in your brain. Serotonin helps regulate how fast or how slow you’ll have a BM. Low serotonin results in loose stools. When you get under stress you further deplete your stress coping chemicals including serotonin. This results in loose stools. The more stress the more likely you are to have a flare up of your irritable bowel symptoms, especially loose stools.
 If you need to increase your dose of magnesium, I would suggest doing so by adding 140 to 150 mg daily (use magnesium citrate or chelate) at dinnertime until you start to see a normal bowel movement. That will be your ideal dose. If you get a loose BM, the reduce your magnesium dose. I have found, however, that the 700 mg in my CFS/Fibro Formula is usually sufficient, but it needs a couple of weeks to start working. If you weight less than one hundred and fifty pounds you might do best taking on pack a day and then supplement your intake of magnesium by an additional 300mg, more if still constipated.
If you need to increase your dose of magnesium, I would suggest doing so by adding 140 to 150 mg daily (use magnesium citrate or chelate) at dinnertime until you start to see a normal bowel movement. That will be your ideal dose. If you get a loose BM, the reduce your magnesium dose. I have found, however, that the 700 mg in my CFS/Fibro Formula is usually sufficient, but it needs a couple of weeks to start working. If you weight less than one hundred and fifty pounds you might do best taking on pack a day and then supplement your intake of magnesium by an additional 300mg, more if still constipated.
It is no secret that prescription medications are dangerous and often life-threatening. They are often removed from the market and then put right back on after stricter laws are in place to regulate the dosage. “Regulating” it, however, does not eliminate the chance of serious side effects, so why not treat this problem naturally and reduce your risks?
If you have IBS I recommend above, magnesium, 5HTP, and digestive enzymes, all contained in my CFS/Fibro Jump Start Package.
Treating the causes of IBS, depleted stress coping chemicals, instead of covering up symptoms with potentially dangerous drugs is always your best approach.





Leave a Reply
Want to join the discussion?Feel free to contribute!